Ambriel vs Assured
Side-by-side comparison to help you choose the right product.
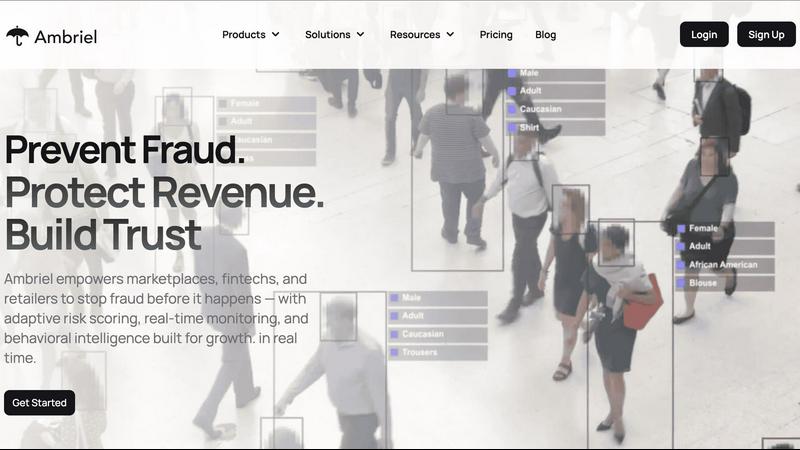
Ambriel uses real time AI to detect and prevent fraud, protecting your revenue and customer trust.
Last updated: March 1, 2026
Assured
Assured uses AI to automate healthcare provider credentialing so you can start billing in days, not months.
Last updated: April 13, 2026
Visual Comparison
Ambriel
Assured
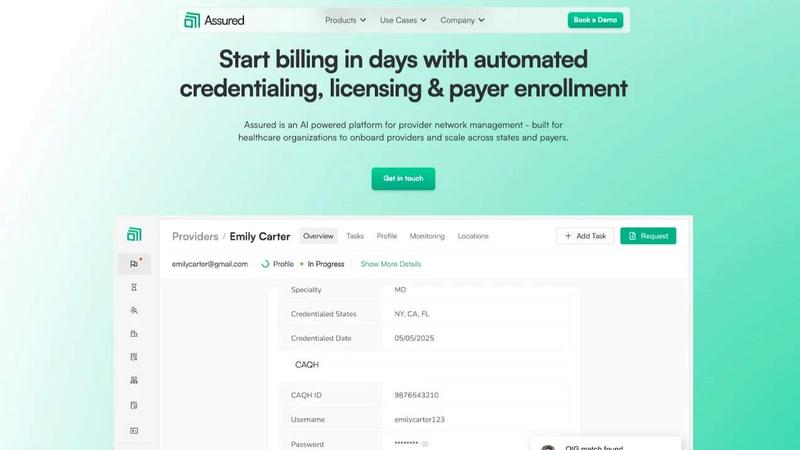
Feature Comparison
Ambriel
Advanced Fraud Detection
This feature uses artificial intelligence to analyze data from over 200 sources to identify suspicious activity as it happens. It assigns a real-time risk score to every user action, such as a login or transaction. This allows businesses to spot complex fraud patterns like synthetic identity creation or payment fraud immediately, enabling them to take action before any financial loss occurs.
Sanctions and PEP Screening
Ambriel automates the critical compliance task of checking users against global watchlists. It screens individuals and entities against over 100 sanctions lists, Politically Exposed Persons (PEP) lists, and crime databases. This removes the need for slow, manual checks, ensuring businesses can meet anti-money laundering (AML) and know-your-customer (KYC) regulations efficiently and without slowing down operations.
Continuous Monitoring
Security is not a one-time event. This feature provides 24/7 surveillance of all user accounts and transactions. It continuously tracks behavior and network signals, looking for unusual patterns that may indicate fraud, such as an account takeover attempt. The system sends alerts on these anomalies, allowing teams to investigate potential threats before they escalate into significant incidents.
Seamless Onboarding
This feature helps businesses build their customer base securely. It allows companies to customize their sign-up and verification processes with automated trust and risk checks. By integrating these checks into the onboarding flow, businesses can efficiently filter out bad actors and bots while ensuring a fast and easy experience for legitimate new customers and sellers.
Assured
AI-Powered Primary Source Verification
This core feature automates the most time-consuming part of credentialing. Instead of staff manually checking each source one by one, Assured's AI simultaneously verifies provider data against a network of over 2,000 primary sources, such as state boards and educational institutions. This parallel processing cuts verification time from weeks down to hours, ensuring data is accurate and audit-ready while dramatically speeding up the entire onboarding timeline.
Automated Payer Enrollment & Tracking
Assured streamlines the complex process of enrolling providers with insurance payers. The platform auto-generates completed applications based on verified data and can submit them directly to payer portals. It then provides real-time tracking for each application, managing follow-ups and alerts for missing requirements. This automation reduces errors, ensures compliance with specific payer rules, and helps organizations get providers in-network approximately 30% faster.
Centralized Provider Data & Network Monitoring
Assured acts as a single source of truth for all provider information. It consolidates data from credentials, licenses, enrollments, and ongoing primary source checks into one unified platform. This centralized roster management allows for real-time monitoring of expirations, sanctions, and other critical changes, providing complete visibility and eliminating surprises during audits. All data formats are supported for seamless integration.
Integrated Licensing Management
Managing state licenses and renewals manually is a major administrative burden, especially for organizations scaling across multiple states. Assured automates this process by tracking license expiration dates, preparing and submitting renewal applications, and handling requirements across all 50 states. This ensures providers remain compliant and able to practice without interruption, removing the hassle and risk from multi-state licensure.
Use Cases
Ambriel
Onboarding and Registration Fraud
During the sign-up process, Ambriel detects and prevents fake accounts, synthetic identities, and automated bot registrations. By analyzing data points from the moment a user tries to create an account, it can block fraudulent actors before they can exploit the platform, protecting marketing budgets and system integrity from the very first interaction.
Payment and Transaction Fraud
This use case focuses on securing financial exchanges. Ambriel monitors every transaction in real-time, spotting anomalies that suggest fraud, such as stolen credit card use or unauthorized transfers. By preventing these fraudulent payments, businesses can avoid direct financial loss, costly chargebacks, and damage to their relationships with payment processors.
Bonus and Promotion Abuse
Businesses use promotions to attract customers, but these can be exploited. Ambriel identifies and stops abuse of incentive programs, such as users creating multiple accounts to claim a sign-up bonus repeatedly or engaging in referral scams. This ensures marketing spend rewards genuine customers and maintains fair play.
Account Takeover Protection
This use case safeguards existing user accounts. Ambriel identifies unusual login behavior, such as attempts from new devices or locations, and detects credential stuffing attacks. By flagging these activities, it helps prevent unauthorized access, keeping customer accounts, data, and funds secure from compromise.
Assured
Accelerating Growth for Digital Health Companies
Digital health startups and companies expanding into new markets need to onboard providers rapidly to meet patient demand and generate revenue. Assured automates the credentialing and enrollment bottleneck, enabling these companies to move providers from application to seeing patients in less than a month. This speed is critical for scaling operations across dozens of states without being stalled by administrative paperwork.
Streamlining Multi-State Expansion for Provider Groups
When a specialty provider group, such as a dermatology or telehealth practice, decides to expand its services into new states, it faces a mountain of varying state licensing and payer rules. Assured provides the deep state-by-state expertise and automation to navigate this complexity from a single platform, credentialing and enrolling providers in weeks instead of months, so patients can access care without delay.
Ensuring Compliance and Audit Readiness for Health Systems
Large health systems and hospitals must maintain rigorous, up-to-date records for hundreds or thousands of providers to pass audits and maintain accreditation. Assured's continuous monitoring from primary sources and centralized data hub ensures all provider information is automatically verified and current, providing peace of mind and a defensible audit trail without manual effort.
Optimizing Network Management for Payers and IPAs
Insurance payers and Independent Practice Associations (IPAs) manage vast provider networks and need efficient tools to onboard new providers and monitor existing ones. Assured gives them clear visibility into every step of the enrollment process and automates ongoing data checks, enabling faster network growth and proactive management of provider compliance and status changes.
Overview
About Ambriel
Ambriel is a foundational fraud intelligence and risk management platform designed for digital businesses. At its core, it provides the essential tools needed to operate securely and maintain regulatory compliance. The platform is built for industries where trust and security are paramount, including fintech, online marketplaces, retail, and iGaming. Its primary purpose is to protect a business's revenue and reputation by identifying and stopping fraudulent activity before it causes harm. Ambriel achieves this by integrating several key security functions into one system: behavioral analytics, device intelligence, sanctions screening, and real-time risk scoring. This integration allows it to analyze transactions, user behaviors, and network signals to uncover hidden risk patterns. The main value proposition of Ambriel is its ability to automate the detection and mitigation of fraud without creating unnecessary barriers for legitimate customers. This means businesses can build trust and ensure safety while keeping the user experience smooth and frictionless for genuine users.
About Assured
Assured is an AI-powered provider network management platform designed to solve a fundamental problem in healthcare administration: the slow, manual, and error-prone processes that delay revenue and hinder growth. It serves as a centralized system for healthcare organizations to manage the entire lifecycle of a provider's network participation. This includes the critical tasks of credentialing, licensing, payer enrollment, and ongoing data monitoring. Built for provider groups, health systems, payers, and digital health companies, Assured addresses the core issue of disconnected data spread across outdated systems. Its primary value proposition is replacing weeks of manual work with automated, parallelized processes powered by artificial intelligence. As an NCQA-certified Credentials Verification Organization (CVO), Assured leverages its authority and technology to verify provider credentials across over 2,000 primary sources simultaneously. The result is a dramatic increase in speed and accuracy, enabling organizations to credential providers in as little as 48 hours instead of 60+ days, achieve 95% first-pass approval rates for payer enrollments, and detect compliance issues much earlier. Ultimately, Assured helps healthcare organizations scale efficiently, reduce administrative costs, start billing faster, and maintain continuous compliance with real-time oversight.
Frequently Asked Questions
Ambriel FAQ
What types of fraud can Ambriel detect?
Ambriel is designed to identify a wide range of fraudulent activities common in digital business. This includes synthetic identity creation, payment fraud, money laundering, bonus and promotion abuse, multi-accounting, referral fraud, and account takeover attempts. Its system analyzes patterns across user behavior, devices, and transactions to spot these threats.
How does Ambriel help with regulatory compliance?
The platform provides automated tools essential for compliance. Its core screening feature checks users against global sanctions, PEP, and watchlists, which is a fundamental requirement for Anti-Money Laundering (AML) programs. Furthermore, its infrastructure and data handling are built to support standards like GDPR, helping businesses meet key legal obligations.
Does Ambriel slow down the user experience for legitimate customers?
A primary goal of Ambriel is to protect without adding friction. Its risk scoring and checks are designed to run in the background seamlessly. For the vast majority of legitimate users, these processes are invisible and do not interrupt their journey, allowing for both high security and a smooth customer experience.
Which industries is Ambriel best suited for?
Ambriel is tailored for digital-first industries that handle online transactions and user registrations. Its key verticals include financial technology (fintech), online marketplaces, e-commerce retail, iGaming, cryptocurrency platforms, and insurance. Any business that needs to manage online risk and build digital trust can benefit from its features.
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Traditional credentialing is a sequential, manual process that can take 60 to 180 days. Assured reduces this to as little as 48 hours by using AI to perform verifications across 2,000+ primary sources in parallel and automating application generation. This efficiency saves organizations significant labor costs, estimated between $4,200 and $5,800 per provider annually, by reclaiming dozens of administrative hours per week.
What makes Assured more reliable than manual credentialing processes?
Assured's reliability stems from its NCQA-CVO certification, which signifies the highest standard for verification accuracy, and its AI-driven automation. Manual processes are prone to human error, delays, and oversight. Assured ensures consistent, thorough checks and eliminates errors in data entry and follow-up, leading to a 95% first-pass approval rate for payer enrollments and earlier detection of critical issues like sanctions.
Can Assured integrate with our existing software systems?
Yes, Assured is built for integration. It offers plug-and-play APIs that allow it to connect seamlessly with your existing technology stack, including Applicant Tracking Systems (ATS), Electronic Medical Records (EMR), and CRM platforms like Salesforce. This ensures data flows smoothly between systems without the need for duplicate entry or disruptive changes to your current workflow.
How does Assured handle ongoing compliance and monitoring after a provider is onboarded?
Onboarding is just the beginning. Assured provides continuous network management by automatically monitoring all verified primary sources for any changes to a provider's status, such as license expirations, new sanctions, or malpractice claims. The platform sends real-time alerts, allowing your team to address issues proactively, often 22 days earlier than manual methods, ensuring ongoing compliance and audit readiness.
Alternatives
Ambriel Alternatives
Ambriel is a fraud intelligence and risk management platform. It falls into the category of business productivity and management software, specifically designed to protect digital revenue. It helps companies in sectors like fintech and e-commerce detect and prevent fraudulent transactions in real time. Businesses often look for alternatives to such platforms for several practical reasons. The primary considerations usually involve pricing and budget constraints, as these solutions can represent a significant investment. Other factors include the specific feature set required, the need for integration with existing business systems, or a preference for a different user experience or customer support model. When evaluating any alternative, focus on the core capabilities that protect your business. Essential aspects to compare include the accuracy of real-time fraud detection, the depth of compliance screening for sanctions, the flexibility of the onboarding process, and the overall reliability of the platform. The right choice effectively balances robust security with a smooth experience for your legitimate customers.
Assured Alternatives
Assured is an AI-powered platform in the provider network management category. It automates credentialing and payer enrollment, helping healthcare organizations reduce administrative delays and start billing faster. Users may look for alternatives for various reasons. These can include budget constraints, the need for different feature sets, or specific platform requirements like deeper integration with existing practice management software. The scale of an organization also plays a key role in this decision. When evaluating options, focus on core capabilities. Key considerations are the automation level for credentialing and enrollment, the accuracy and speed promised, compliance certifications like NCQA-CVO status, and the platform's ability to provide real-time monitoring and centralized data management.