Assured vs incentX
Side-by-side comparison to help you choose the right product.
Assured
Assured uses AI to automate healthcare provider credentialing so you can start billing in days, not months.
Last updated: April 13, 2026
incentX automates accurate incentive payouts using precise transaction data.
Last updated: February 28, 2026
Visual Comparison
Assured
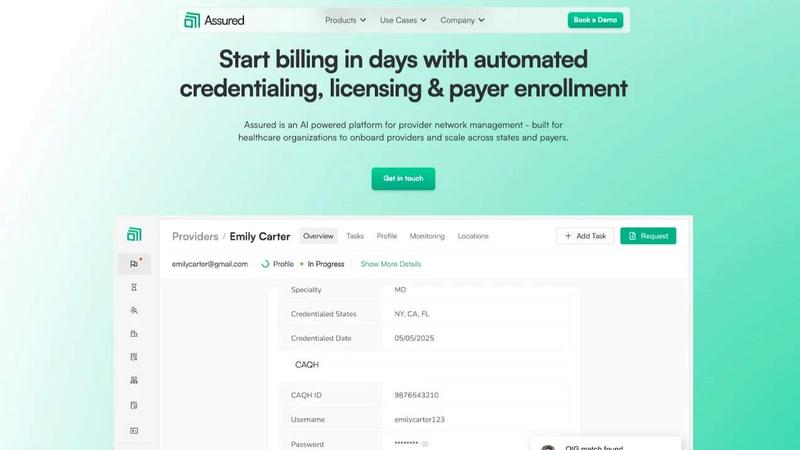
incentX
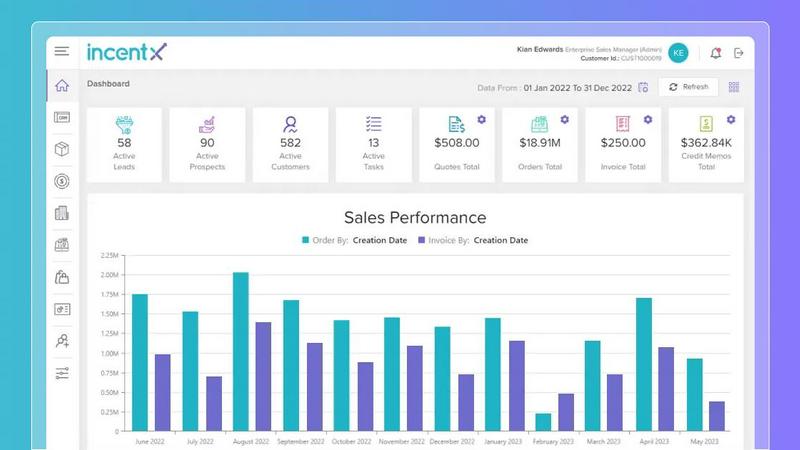
Feature Comparison
Assured
AI-Powered Primary Source Verification
This core feature automates the most time-consuming part of credentialing. Instead of staff manually checking each source one by one, Assured's AI simultaneously verifies provider data against a network of over 2,000 primary sources, such as state boards and educational institutions. This parallel processing cuts verification time from weeks down to hours, ensuring data is accurate and audit-ready while dramatically speeding up the entire onboarding timeline.
Automated Payer Enrollment & Tracking
Assured streamlines the complex process of enrolling providers with insurance payers. The platform auto-generates completed applications based on verified data and can submit them directly to payer portals. It then provides real-time tracking for each application, managing follow-ups and alerts for missing requirements. This automation reduces errors, ensures compliance with specific payer rules, and helps organizations get providers in-network approximately 30% faster.
Centralized Provider Data & Network Monitoring
Assured acts as a single source of truth for all provider information. It consolidates data from credentials, licenses, enrollments, and ongoing primary source checks into one unified platform. This centralized roster management allows for real-time monitoring of expirations, sanctions, and other critical changes, providing complete visibility and eliminating surprises during audits. All data formats are supported for seamless integration.
Integrated Licensing Management
Managing state licenses and renewals manually is a major administrative burden, especially for organizations scaling across multiple states. Assured automates this process by tracking license expiration dates, preparing and submitting renewal applications, and handling requirements across all 50 states. This ensures providers remain compliant and able to practice without interruption, removing the hassle and risk from multi-state licensure.
incentX
Transaction-Level Calculation Engine
At its core, incentX automates calculations by tying every incentive directly to granular transaction data from your ERP system. This means commissions are based on actual fulfilled orders, rebates on real claims, and royalties on confirmed sales—not estimates or forecasts. This engine applies complex rules and filters (by product, region, margin, etc.) to this data, ensuring every payout is precise and traceable back to its source, eliminating guesswork and manual errors.
Real-Time Forecasting & Visibility
The platform provides predictive insights by using live transaction data to forecast future payouts. You can model costs by product, team, or region based on actual margin and fulfillment pipelines, not sales guesses. This gives finance and operations leaders clear visibility into upcoming incentive liabilities, enabling accurate budgeting and preventing costly overpayments or last-minute financial adjustments.
Unified Incentive Management Suite
incentX consolidates multiple incentive types—sales commissions, partner rebates, royalties, and vendor chargebacks—into one centralized platform. Instead of managing separate, disconnected tools for each program, all incentives run from the same transaction-level data foundation. This provides a holistic view of your total incentive spend and ensures consistency and accuracy across all your revenue programs.
Transparent Stakeholder Portal
The platform offers clear visibility to all participants, such as sales representatives and partners. They can see the exact transactions behind their earnings, understanding how each commission line item or rebate was calculated. This transparency drastically reduces administrative back-and-forth and disputes, as everyone has access to the same auditable data, building trust in the compensation process.
Use Cases
Assured
Accelerating Growth for Digital Health Companies
Digital health startups and companies expanding into new markets need to onboard providers rapidly to meet patient demand and generate revenue. Assured automates the credentialing and enrollment bottleneck, enabling these companies to move providers from application to seeing patients in less than a month. This speed is critical for scaling operations across dozens of states without being stalled by administrative paperwork.
Streamlining Multi-State Expansion for Provider Groups
When a specialty provider group, such as a dermatology or telehealth practice, decides to expand its services into new states, it faces a mountain of varying state licensing and payer rules. Assured provides the deep state-by-state expertise and automation to navigate this complexity from a single platform, credentialing and enrolling providers in weeks instead of months, so patients can access care without delay.
Ensuring Compliance and Audit Readiness for Health Systems
Large health systems and hospitals must maintain rigorous, up-to-date records for hundreds or thousands of providers to pass audits and maintain accreditation. Assured's continuous monitoring from primary sources and centralized data hub ensures all provider information is automatically verified and current, providing peace of mind and a defensible audit trail without manual effort.
Optimizing Network Management for Payers and IPAs
Insurance payers and Independent Practice Associations (IPAs) manage vast provider networks and need efficient tools to onboard new providers and monitor existing ones. Assured gives them clear visibility into every step of the enrollment process and automates ongoing data checks, enabling faster network growth and proactive management of provider compliance and status changes.
incentX
Automating Complex Sales Commissions
For companies with multi-tiered, performance-based sales plans, incentX automates the entire commission lifecycle. It calculates payouts using real revenue and margin data from fulfilled orders, aligns compensation with strategic goals like profitability, and provides reps with real-time dashboards. This use case eliminates spreadsheet chaos, ensures reps are paid accurately and on time, and allows managers to adjust plans dynamically based on actual performance data.
Streamlining Partner & Channel Rebate Programs
Manufacturers and distributors use incentX to manage complex rebate agreements with their channel partners. The platform automates the tracking of order volumes and claims against agreed-upon tiers directly from ERP data. This eliminates "shadow accounting," ensures rebates are calculated accurately and paid promptly, and provides both the company and its partners with a clear, shared view of program performance and earnings.
Ensuring Accurate Royalties Management
For businesses that license intellectual property or brands, incentX calculates royalty payments based on actual sales data, not estimates. It pulls transaction details from the ERP to determine exactly what was sold, where, and at what price, applying the correct royalty rate. This creates an audit-ready trail, ensures licensors are paid fairly, and helps licensees accurately forecast their royalty expenses.
Managing Vendor Chargebacks & Deductions
Retailers and distributors use incentX to efficiently manage chargebacks from vendors for issues like shipping errors or damaged goods. The platform matches every vendor deduction to the specific transaction and invoice in the ERP system. This provides full visibility into the reason for each chargeback, streamlines the reconciliation process, and ensures disputes are resolved quickly and based on factual data.
Overview
About Assured
Assured is an AI-powered provider network management platform designed to solve a fundamental problem in healthcare administration: the slow, manual, and error-prone processes that delay revenue and hinder growth. It serves as a centralized system for healthcare organizations to manage the entire lifecycle of a provider's network participation. This includes the critical tasks of credentialing, licensing, payer enrollment, and ongoing data monitoring. Built for provider groups, health systems, payers, and digital health companies, Assured addresses the core issue of disconnected data spread across outdated systems. Its primary value proposition is replacing weeks of manual work with automated, parallelized processes powered by artificial intelligence. As an NCQA-certified Credentials Verification Organization (CVO), Assured leverages its authority and technology to verify provider credentials across over 2,000 primary sources simultaneously. The result is a dramatic increase in speed and accuracy, enabling organizations to credential providers in as little as 48 hours instead of 60+ days, achieve 95% first-pass approval rates for payer enrollments, and detect compliance issues much earlier. Ultimately, Assured helps healthcare organizations scale efficiently, reduce administrative costs, start billing faster, and maintain continuous compliance with real-time oversight.
About incentX
incentX is a comprehensive incentive automation platform built on a simple, powerful idea: pay people based on what actually happens in your business. It moves companies away from error-prone spreadsheets and disconnected systems by connecting directly to the core systems that track real transactions—your CRM and ERP. This foundational connection allows incentX to calculate sales commissions, partner rebates, royalties, and other incentives with precision, using fulfilled orders, real margins, and actual sales data. The platform is designed for revenue, finance, and operations teams in organizations where incentive complexity has outgrown manual processes. Its core value is creating a single, audit-ready source of truth for all incentive programs. This eliminates costly disputes, prevents forecasting surprises, and ensures that every payout is accurate, justified, and drives the right business behaviors. By automating what was once a manual, IT-heavy burden, incentX gives teams real-time visibility and control, turning incentive management from a administrative headache into a strategic asset for profitable growth.
Frequently Asked Questions
Assured FAQ
How does Assured reduce provider onboarding time and administrative costs?
Traditional credentialing is a sequential, manual process that can take 60 to 180 days. Assured reduces this to as little as 48 hours by using AI to perform verifications across 2,000+ primary sources in parallel and automating application generation. This efficiency saves organizations significant labor costs, estimated between $4,200 and $5,800 per provider annually, by reclaiming dozens of administrative hours per week.
What makes Assured more reliable than manual credentialing processes?
Assured's reliability stems from its NCQA-CVO certification, which signifies the highest standard for verification accuracy, and its AI-driven automation. Manual processes are prone to human error, delays, and oversight. Assured ensures consistent, thorough checks and eliminates errors in data entry and follow-up, leading to a 95% first-pass approval rate for payer enrollments and earlier detection of critical issues like sanctions.
Can Assured integrate with our existing software systems?
Yes, Assured is built for integration. It offers plug-and-play APIs that allow it to connect seamlessly with your existing technology stack, including Applicant Tracking Systems (ATS), Electronic Medical Records (EMR), and CRM platforms like Salesforce. This ensures data flows smoothly between systems without the need for duplicate entry or disruptive changes to your current workflow.
How does Assured handle ongoing compliance and monitoring after a provider is onboarded?
Onboarding is just the beginning. Assured provides continuous network management by automatically monitoring all verified primary sources for any changes to a provider's status, such as license expirations, new sanctions, or malpractice claims. The platform sends real-time alerts, allowing your team to address issues proactively, often 22 days earlier than manual methods, ensuring ongoing compliance and audit readiness.
incentX FAQ
What core business systems does incentX integrate with?
incentX is built to integrate directly with your company's foundational systems. Its primary connections are with Enterprise Resource Planning (ERP) systems, such as SAP or Oracle, to access real transaction, order, and fulfillment data. It also integrates with Customer Relationship Management (CRM) platforms like Salesforce to incorporate sales pipeline and performance data. This seamless integration is what powers its accurate, transaction-level calculations.
How does incentX reduce disputes over commissions or rebates?
It reduces disputes through unparalleled transparency and data accuracy. Since all calculations are rooted in actual transactions from your ERP, every payout can be traced back to the specific orders, invoices, and line items that generated it. Sales reps and partners have direct visibility into this data through their portals, so they can see exactly how their earnings were calculated, removing ambiguity and building trust.
Is incentX only for managing sales team commissions?
No, incentX is designed as a complete incentive management suite. While it robustly handles sales compensation, its transaction-based engine is equally powerful for managing buy-side incentives. This includes partner and customer rebates, royalty agreements, trade promotions, and vendor chargebacks. It provides a single platform to oversee all incentive spending, both on the sales and procurement sides of your business.
How does the platform help with financial planning and forecasting?
incentX transforms forecasting from an educated guess into a data-driven process. By linking forecast models to the pipeline of real, fulfilled transactions in your ERP, it can predict future payouts with high accuracy. Finance teams can forecast incentive costs by product line, sales region, or team based on actual margins and order volumes, leading to more reliable budgets and cash flow projections.
Alternatives
Assured Alternatives
Assured is an AI-powered platform in the provider network management category. It automates credentialing and payer enrollment, helping healthcare organizations reduce administrative delays and start billing faster. Users may look for alternatives for various reasons. These can include budget constraints, the need for different feature sets, or specific platform requirements like deeper integration with existing practice management software. The scale of an organization also plays a key role in this decision. When evaluating options, focus on core capabilities. Key considerations are the automation level for credentialing and enrollment, the accuracy and speed promised, compliance certifications like NCQA-CVO status, and the platform's ability to provide real-time monitoring and centralized data management.
incentX Alternatives
incentX is a specialized software platform in the business and finance category, designed to automate incentive compensation. It centralizes the calculation of sales commissions, rebates, and royalties by using precise transaction data from your core business systems. This approach replaces manual spreadsheets to ensure accuracy and efficiency. Businesses explore alternatives to incentX for several fundamental reasons. Common motivations include budget constraints, where the cost may not align with a company's current size or needs. Others may require a different set of features, a simpler tool for less complex programs, or a platform that integrates with a specific niche software their operations depend on. When evaluating any alternative, focus on core capabilities. The essential factors are accurate, automated calculations, seamless integration with your existing CRM and ERP data, and clear visibility into payout forecasts. The right tool should eliminate spreadsheet reliance, reduce payment disputes, and provide a reliable, audit-ready record of all incentive transactions.